Our Blog

Our
Blog
Avoid Getting Sick for Christmas
Are you noticing how everyone around you seems to be sick right now? I don’t want my patients to be worried or sick over the holidays, so here is an updated protocol for all the winter bugs. The idea is to get your immune system strong, so you are able to resist or...
Glutathione: A Most Powerful Antioxidant
Glutathione plays an extremely important role in protecting liver cells, red blood cells, and many other types of cells against toxic injury. Made of three amino acids (cysteine, glycine, and glutamine), glutathione functions as a powerful antioxidant. It scavenges...
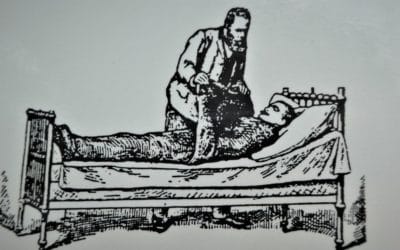
Wet Sheet Wrap to Stimulate Whole Body Circulation
Often used as a method for reducing fevers in adults and children, Wet Sheet Wrap is a form of hydrotherapy that has many uses in natural medicine. Also known as "Spanish Mantel" or "Magic Carpet" (as children like to call it), Wet Sheet Wrap may be used to help...
Don’t Overlook the Health Benefits of Lamb Meat
Lamb meat is a wonderful culinary choice for a wide variety of dishes. With a mild, earthy flavor that takes well to the herbs it is paired with, lamb also contains plenty of nutrients and protein. Folic acid and vitamin B6 are among the many nutrients, as well as the...
Understanding Pyrrole Disorder
One of the essential principles of natural medicine is that the symptoms of illness manifest as a result of underlying or "root" causes. By this, we mean that there is an imbalance in the body which consequently produces symptoms. If we only treat symptoms, as does...
Calendula: Herbal Remedy for the Skin and So Much More
The use of calendula tea, oil, extract, and tincture dates back to ancient Egyptian culture and early Christianity. Calendula (Calendula officinalis) has many health enhancing properties that can help heal inflamed skin, reduce pain and swelling, and support the...
Saffron: A Versatile Medicinal Herb and Culinary Spice
Saffron is an exotic spice native to Southern Europe, but widely used in many cultures around the world for cooking and medicinal purposes. In the kitchen, saffron (Crocus sativus) is used to add vibrant golden color and a sweet, floral and almost nutty flavor to a...
Teens Can Boost their Mental Health Doing Good Deeds
Now that the restrictions of living in pandemic times are lightening, teens have the opportunity to regain their emotional resilience. One way to do this is to encourage your teen to volunteer in their community or at school. They can reap all the health benefits of...
Firecracker Tofu Lettuce Wraps–Your Teens Will Love These!
Teens will love the way the ingredients combine to make the tofu bits crispy and–you guessed it–fiery! Paired with savory brown rice noodles and a creamy sesame sauce, this recipe is sure to awaken your taste buds and make you a tofu fan by the end of the meal!...